Penile Cancer
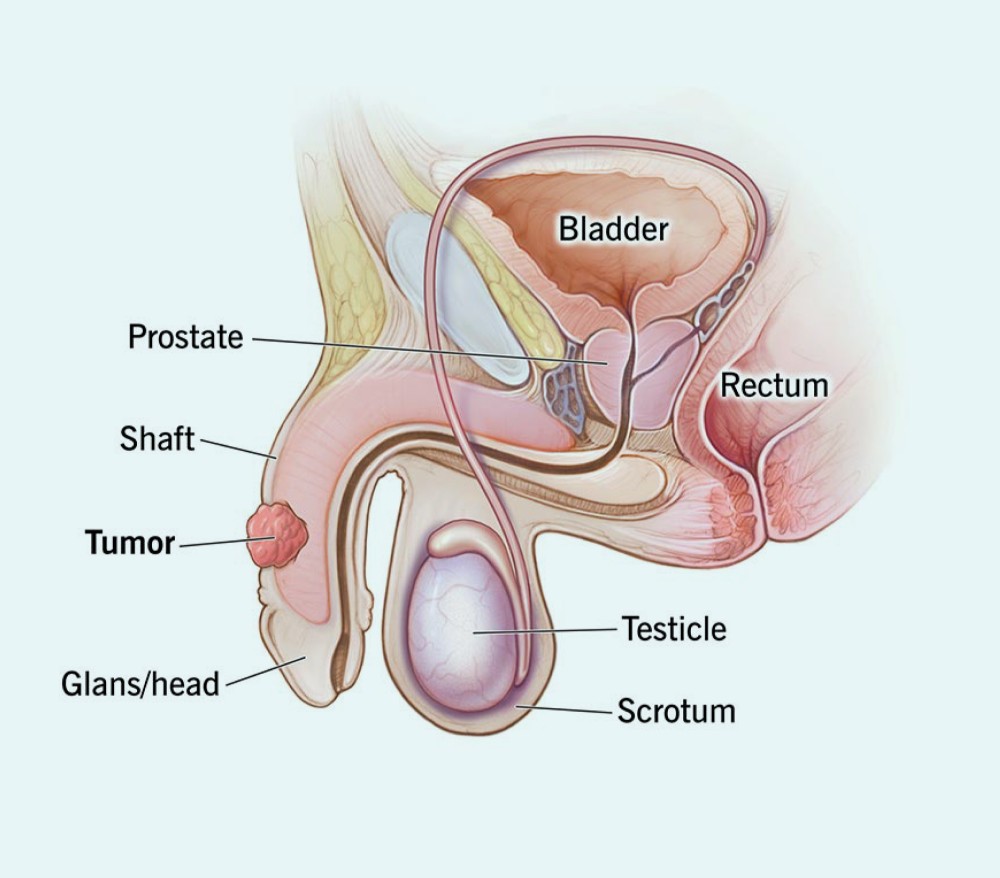
Penile Cancer: Causes, Symptoms, Diagnosis & Treatment
Penile cancer is a rare type of cancer that begins in the tissues of the penis—the external male reproductive organ. The penis is composed of three major tubular structures: two corpora cavernosa (which contain erectile tissue, blood vessels, and nerves) and the corpus spongiosum, which surrounds the urethra and ends in the glans penis.
Penile cancer usually starts as a small lesion, blister, or wart-like growth on the foreskin, head (glans), or shaft of the penis. If left untreated, it may discharge blood or a foul-smelling fluid and can spread to nearby lymph nodes or other organs.
Human papillomavirus (HPV) infection is a key risk factor, but early prevention and hygiene can significantly reduce the chances of developing this disease.
What Causes Penile Cancer?
Several factors may increase the risk of penile cancer, including:
- Poor genital hygiene and conditions like phimosis (inability to retract the foreskin), which allows buildup of smegma.
- HPV infection, especially types 16 and 18, transmitted through unprotected sexual
activity. - HIV/AIDS, which weakens immune response and increases vulnerability to cancers.
- Tobacco use, including smoking and chewing tobacco.
- Chronic balanitis, a persistent inflammation of the glans penis, often in diabetic or immunocompromised patients.
- Lichen sclerosis, a skin condition that can affect the genital area.
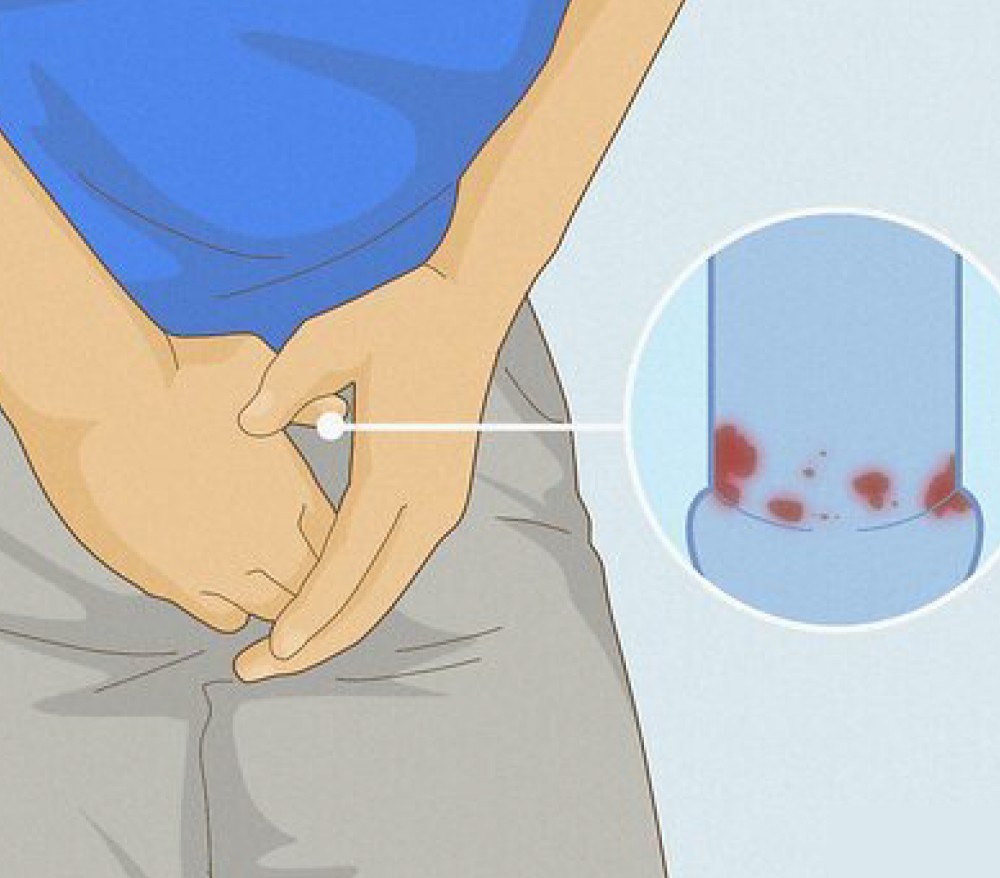
Symptoms of Penile Cancer
Common signs and symptoms include:

Persistent sore or non-healing ulcer on the penis

Swelling of the foreskin or glans (sometimes with foul-smelling discharge)

Lumps or swelling in the groin area
Skin thickening or changes in color of the penile skin

Changes in an existing mole on the penis

Pain or discomfort in the penile region
Early detection is crucial. If you experience any of these symptoms, consult a urologist or cancer specialist promptly.
Types of Penile Cancer
Penile cancer types are classified based on the cell type from which the cancer originates:
- Squamous Cell Carcinoma: Accounts for over 90% of penile cancer cases. Typically starts in the skin cells of the glans or foreskin.
- Basal Cell Carcinoma: A slow-growing type that rarely spreads to other organs.
- Melanoma: Arises from pigment-producing melanocytes and has a high tendency to spread.
- Sarcoma: An aggressive form that originates in the connective or soft tissue of the
penis.

Penile Cancer Prevention
Preventive strategies include:
- Neonatal circumcision, which has been shown to reduce the risk.
- Maintaining proper genital hygiene.
- Using condoms during sexual activity to reduce HPV transmission.
- Avoiding multiple sexual partners.
- Quitting smoking and avoiding tobacco products.
- HPV vaccination, particularly for boys and men, to prevent infection from high-risk HPV strains.
Penile Cancer Diagnosis and Management
To confirm a diagnosis and determine the stage of the disease, doctors may recommend:
Physical Examination
A detailed genital and lymph node examination.
Biopsy
To confirm the cancer type and grade.
Incisional biopsy
For larger lesions, a small tissue sample is removed.
Excisional biopsy
For small growths, the entire lesion is removed.
Lymph Node FNAC
Fine needle aspiration from swollen groin lymph nodes to check for cancer spread.
Imaging Tests
Ultrasound
To detect lymph node enlargement.
CT scan
To assess the spread to pelvic or abdominal organs.
PET-CECT scan
Recommended for advanced or recurrent cases to identify distant metastases.
Treatment Options for Penile Cancer
Treatment depends on the size, type, and spread of the tumor. Options include:
- Performed when small tumours affect only the foreskin (preputial skin).
- Involves surgical removal of the foreskin.
- Considered a minimal and effective intervention for very early-stage disease.
- Recommended for small tumours limited to the glans penis.
- Involves removal of the glans while preserving as much of the remaining penile tissue as possible.
- Helps maintain urinary and sexual function.
- Performed for tumours involving the distal part of the penile shaft.
- Involves removal of the cancerous portion of the penis, preserving a functional penile stump.
- Allows the patient to urinate in a standing position and maintain sexual activity.
- Required for large or extensively spread tumours where a functional penile stump cannot be preserved.
- Involves complete removal of the penis and creation of a new urinary opening (urethrostomy) in the perineum.
- Enables the patient to pass urine comfortably in a seated position.
- Used in very small, early-stage tumours.
- Cancer is removed layer by layer, each examined under a microscope until clear margins are achieved.
- Maximizes tissue preservation and minimizes cosmetic and functional impact.
- Performed when there is evidence or suspicion of groin lymph node involvement.
- May be unilateral or bilateral, depending on the cancer spread.
- Helps reduce the risk of cancer metastasis and assists in staging the disease.
- Reserved for very early cancers or patients unfit for surgery (e.g., elderly or frail).
- Options include:
- Topical agents (e.g., chemotherapy creams)
- Cryotherapy / Cryosurgery
- Laser ablation
- These therapies aim to preserve the penis while effectively managing the disease.
- Given before surgery to reduce tumour size or lymph node involvement.
- Especially useful in locally advanced or node-positive cases to improve surgical outcomes.
- Administered after surgery to eliminate microscopic cancer cells.
- Typically involves 6 cycles, each lasting 2–3 weeks.
- Helps prevent recurrence and control systemic spread.
- Combines chemotherapy with radiation therapy administered simultaneously.
- Enhances the effectiveness of both treatments.
- Used when surgery isn’t possible or to treat advanced local disease.
- Delivers high-energy X-rays or proton beams directly to the tumour site.
- Used in the following settings:
- Primary treatment (alternative to surgery)
- Post-surgical (adjuvant) therapy to minimize recurrence
- Palliative treatment in advanced disease to relieve symptoms
- Offers a non-invasive option with a focus on organ preservation where feasible




