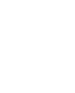Cervical Cancer
Cervical cancer develops in the cervix, which is the lowermost part of the uterus that connects to the vagina. In most cases, cervical cancer is caused by persistent infection with Human Papilloma Virus (HPV), which is a viral infection, acquired through sexual contact.
Presently, vaccines to prevent HPV infection are available for teenagers’ and young adults; also routine screening of sexually active women can help detect those women with persistent HPV infection and timely treatment can prevent infected cells to transform into cancerous cells.
Symptoms of Cervix Cancer:
Early-stage cervical cancer generally does not show any signs or symptoms. Some of the most common symptoms that patients present to the doctor are:
After it spreads to other parts, the symptoms may include:

Diagnostics Facilities
Advanced Cancer Diagnostics
Advanced Cancer Treatment
General Diagnostic Facilities
Causes of Cervix Cancer
Although the causes of cervix cancer are not known definitely, it is suggested that infection with HPV, i.e. Human Papilloma Virus plays a crucial role and is very common in women who have cervix cancer. The risk factors that are known to be associated with cervix cancer are as follows:
- A high number of sexual partners increase the chances of acquiring HPV infection.
- Sexual activities at an early age increase the chances of contracting the virus.
- Poor genital hygiene
- Exposure to STDs (Sexually Transmitted Diseases) like HIV (Human Immunodeficiency Virus), Chlamydia, Gonorrhea, or Syphilis can also increase the risk.
- Autoimmune diseases, a weak immune system due to constant exposure to infections or immune suppressants triggers cervical cancer.
- Smoking
- Changes in progesterone hormone levels
When to see the doctor?
It is best to consult our specialist at the earliest if you frequently experience any of these problems or symptoms mentioned above.
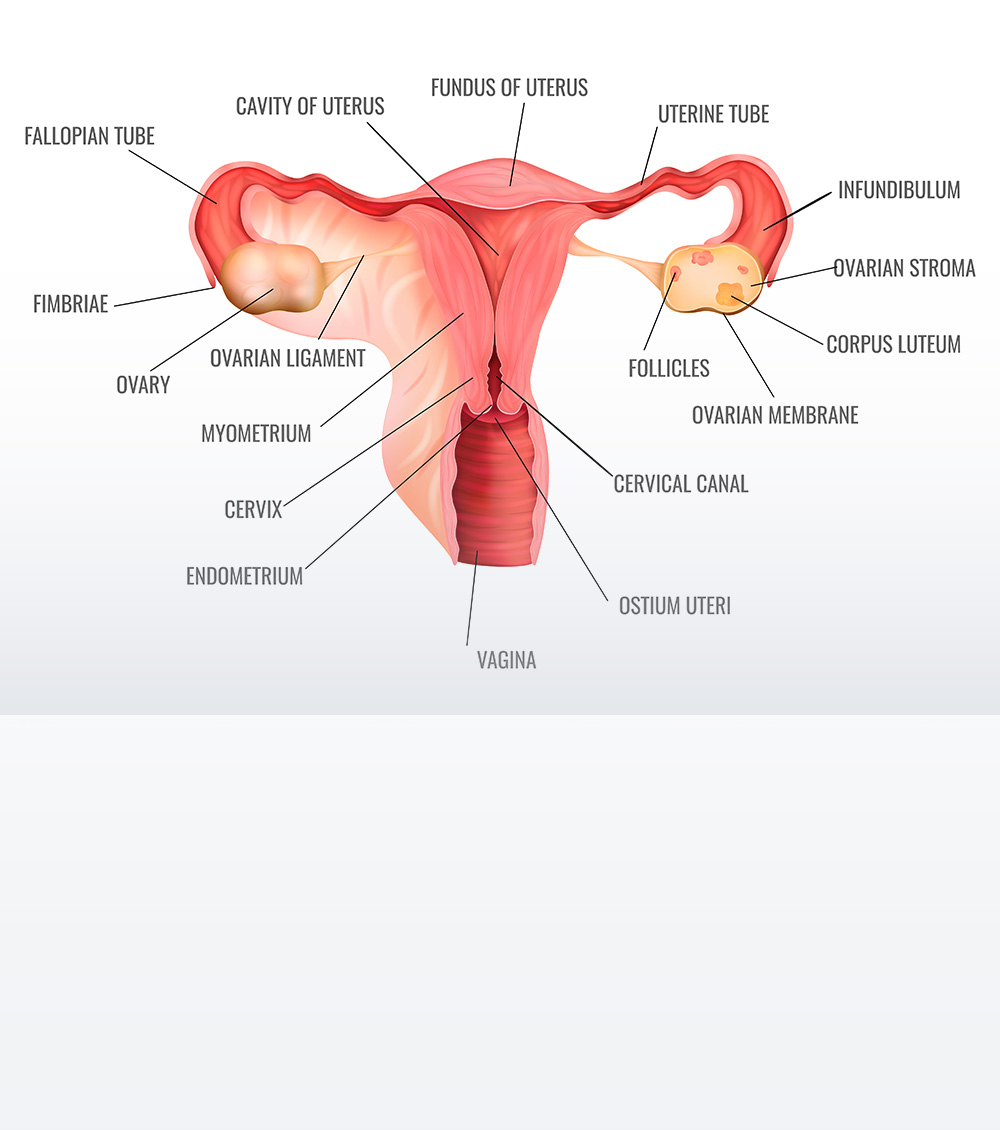
Prevention of Cervix Cancer
- Having protected sex
- Not having too many sexual partners
- Adopting healthy lifestyles
- HPV vaccination
HPV Vaccine
HPV vaccines can be taken from the age of 9 to 25 years after consultation with your doctor, and their dosage varies with age.
These vaccines work like other immunization processes and guard against viral infections by stimulating the body to produce antibodies which encounter HPV infections in the future by binding to the virus and preventing it from infecting healthy cells.
HPV vaccines do not prevent other sexually transmitted diseases and do not treat existing HPV infections or other HPV-related diseases.
Investigative tests to do for Cervical Cancer
The following tests are used to screen and diagnose cervical cancer:
- Pelvic exam: This is a non-invasive preliminary exam requiring only a few minutes wherein the vulva, cervix, vagina, uterus, ovaries and other organs are examined using the speculum and can be performed easily in the outpatient department. In case of any unusual findings, our consultant might recommend the following tests to arrive at a definitive diagnosis:
- PAP smear: A PAP smear is done when the consultant has suspicions about the presence of cancer and no obvious lesion, wherein he gently scrapes the outer layer cells from your cervix and vagina for further testing and the following tests are done after a PAP test:
- Thinprep or Surepath test: The liquid-based cytology test transfers a thin layer of cells onto a slide after removing blood or mucus from the sample.
- Auto Cpap or Focal point: A computer screens the sample to detect abnormal cells.
- Colposcopy: The doctor uses a special magnifying instrument to check the cervix for abnormalities. It magnifies and illuminates the cells of the cervix and vagina and can also be used to perform a cervix biopsy.
- Biopsy: A small amount of tissue from the cervix is taken for examination under a microscope, which enables a definite diagnosis.
- HPV typing: This test is done to detect the presence of Human Papilloma Viruses like HPV 16 and HPV 18, whose infection causes cervix cancer.
- CT scan: A Computerised tomography of a patient provides a 3D visual image of the tumour size, position and spread. Contrast CT is done by injecting a dye which gives finer visuals and details of the tumour.
- MRI: Magnetic Resonance Imaging uses magnetic fields to produce a detailed visual image of the tumour.
- Positron Emission Tomography: The cancer cells in the body absorb the short-acting radioactive glucose injected into the patient, which lights up the area and can be detected using sensitive devices to determine the exact position, size and spread of the tumour.
- Precancerous Lesions: Cervical cancer does not develop in a short period. They start as pre-cancerous lesions. Studies have shown that it takes more than a decade for a pre-cancerous lesion to develop into cervical cancer. During this period of development, it is easy to identify these lesions by screening procedures and get treated early even before the cancer develops.

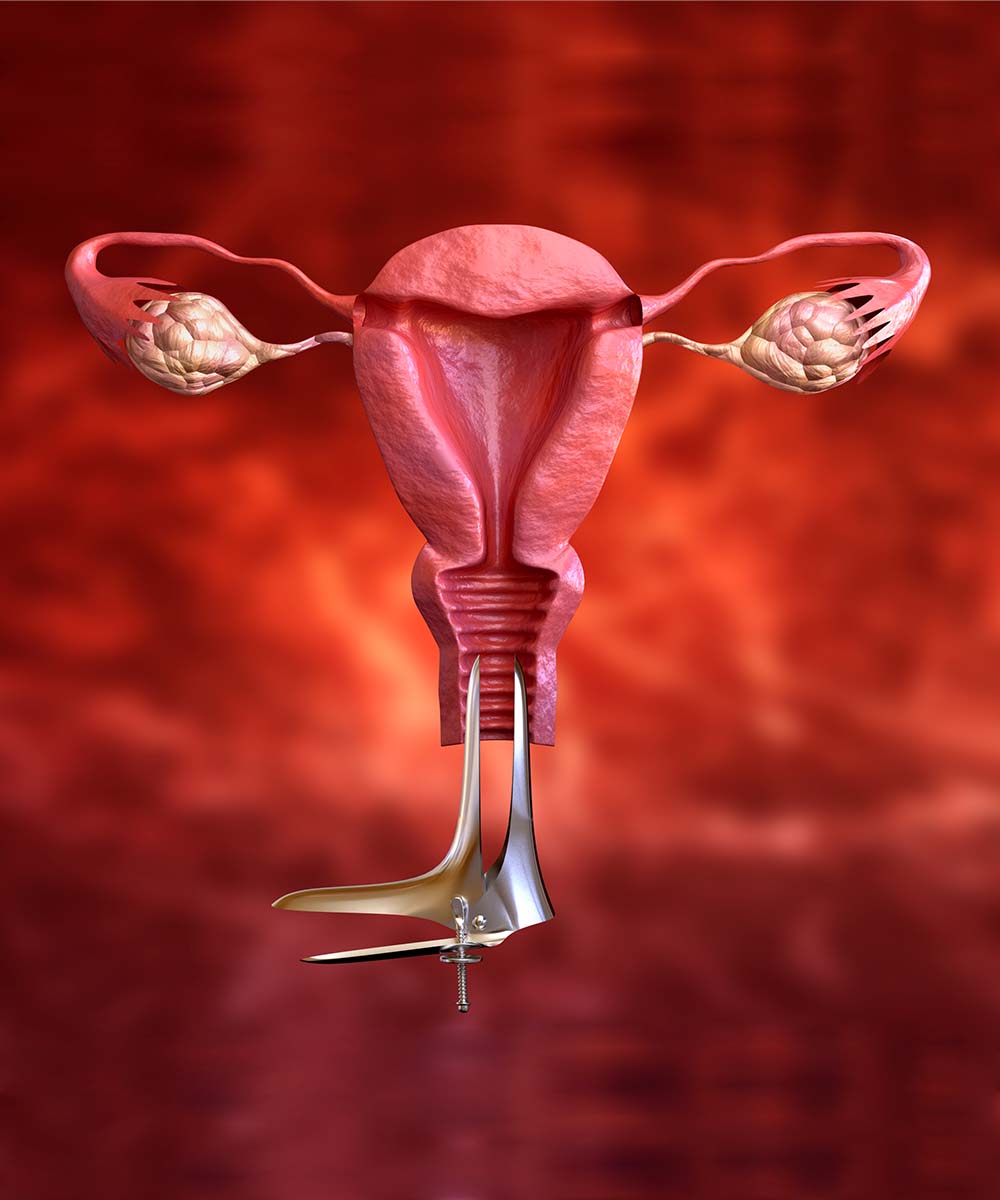
Treatment for Cervical Cancer
Treatment approaches for cervical cancer depend on the tumour’s size and spread, histology, disease staging, patient’s general health condition and associated diseases.
Doctors determine the appropriate treatment strategy which comprises surgery, chemotherapy or radiotherapy in different combinations or given individually based on patient health needs.
Surgery:
- Patients with precancerous lesions undergo a small surgical procedure called LEEP (Loop Electrosurgical Excision Procedure) wherein an electric current heated wire loop is used to remove cells from the cervical region.
- If the tumour area is relatively small fertility sparring approach is preferred and Trachelectomy surgery is performed.
- A hysterectomy is performed wherein the patient’s uterus is removed along with the adjoining lymph nodes when cancer has spread into the uterus. In elderly patients, who have attained menopause, the ovaries are also removed.
Radiation Therapy:
- When the tumour is large or the cancer has spread beyond the uterus, radiation therapy with or without chemotherapy is adopted to treat cancer.
- High-energy X-ray beams are targeted on the cancerous areas to destroy malignant cells and inhibit their growth.
- Radiation treatment may be external or internal (brachytherapy) and affects only the local site of treatment.
- In external beam radiation therapy, the energy beams are aimed at the pelvis with the help of a Linear Accelerator using advanced techniques like 3DCRT, IMRT, IGRT or Rapid-Arc.
- In brachytherapy, radiation is emitted from a radioactive seed which is inserted into the patient’s cervix and uterus using brachytherapy applicators.
- Radiotherapy is also given as palliative therapy in very advanced cancers where the disease has spread beyond the pelvic region to other organs like the liver, bone and brain to relieve symptoms like bleeding, bone pain or CNS symptoms.
Chemotherapy:
- In chemotherapy, oral medications are used to eliminate cancer cells; the intensive treatment is continuously given in cycles (usually weekly) with a short recovery period in-between.
- In metastatic cancers where the tumours have spread beyond the local region, chemotherapy is given as a palliative treatment.
Doctors

Dr. Deepti Mishra

Dr. Aruna Prabhu

Dr. Bhavesh Poladia

Dr. Karthick Rajamanickam