Skin Cancer
Our skin consists of three layers the epidermis, the top layer of the skin protects our body and is thin in some regions and thicker in other places. The second layer called the dermis is thicker than the epidermis, consisting of the sweat glands (which cools our body), nerve endings (enabling a sense of touch, temperature, and pressure), hair roots & oil glands (keep the skin moist) and blood vessels (to supply nutrition to the skin). The third and lowermost layer of the skin is the subcutaneous fat layer, which attaches the skin to the body, helping control body temperature and acting as a fat reserve.
The abnormal and uncontrolled growth of cells usually happens in the epidermis, the outermost layer of our skin. Mutations are triggered due to the deterioration of the DNA, often due to high exposure of skin to sunrays and in some cases on areas of skin not ordinarily exposed to sunlight and lead to the formation of cancer cells on the skin.
Symptoms of Skin Cancer:
Different types of skin cancers may exhibit different symptoms.

Diagnostics Facilities
Advanced Cancer Diagnostics
Advanced Cancer Treatment
General Diagnostic Facilities
Causes of Skin Cancer
- Exposure to UV Radiation: The ultraviolet radiation found in the sun or tanning beds can be harmful to the skin, resulting in DNA damage. Going out in the sun for long periods without a protective cover (clothes or sunscreens) can increase the risk. Having sunburns mean that your skin is not able to protect itself from the sun, which puts you at a higher risk of cancer than others.
- Fair Skin: Melanin (the pigment responsible for skin colour) protects the skin from UV rays; skin cancer can occur in any individual irrespective of skin colour, and lighter skin increases the risk of skin cancer.
- Moles:If you have moles of irregular shape and an unusual number of moles, you may be at a higher risk for cancer.
- Precancerous skin lesions: Skin lesions known as actinic keratoses can increase your risk of developing skin cancer. These precancerous skin growths typically appear as rough, scaly patches varying in colour from brown to dark pink and are typically found on the face, head and hands of fair-skinned people whose skin has been damaged by UV rays from sunlight.
- Family History:Having a positive family history of skin cancer, can increase your risk of getting skin cancer.
- Weak immune system: People with weakened immune systems have a greater risk of developing skin cancer, which includes individuals with HIV/AIDS or taking immunosuppressant drugs after an organ transplant.
- Radiation exposure:People who received radiation treatment for skin conditions such as eczema and acne may have an increased risk of skin cancer, particularly basal cell carcinoma.
- Exposure to certain substances:Exposure to certain substances, such as arsenic, may increase your risk of skin cancer.
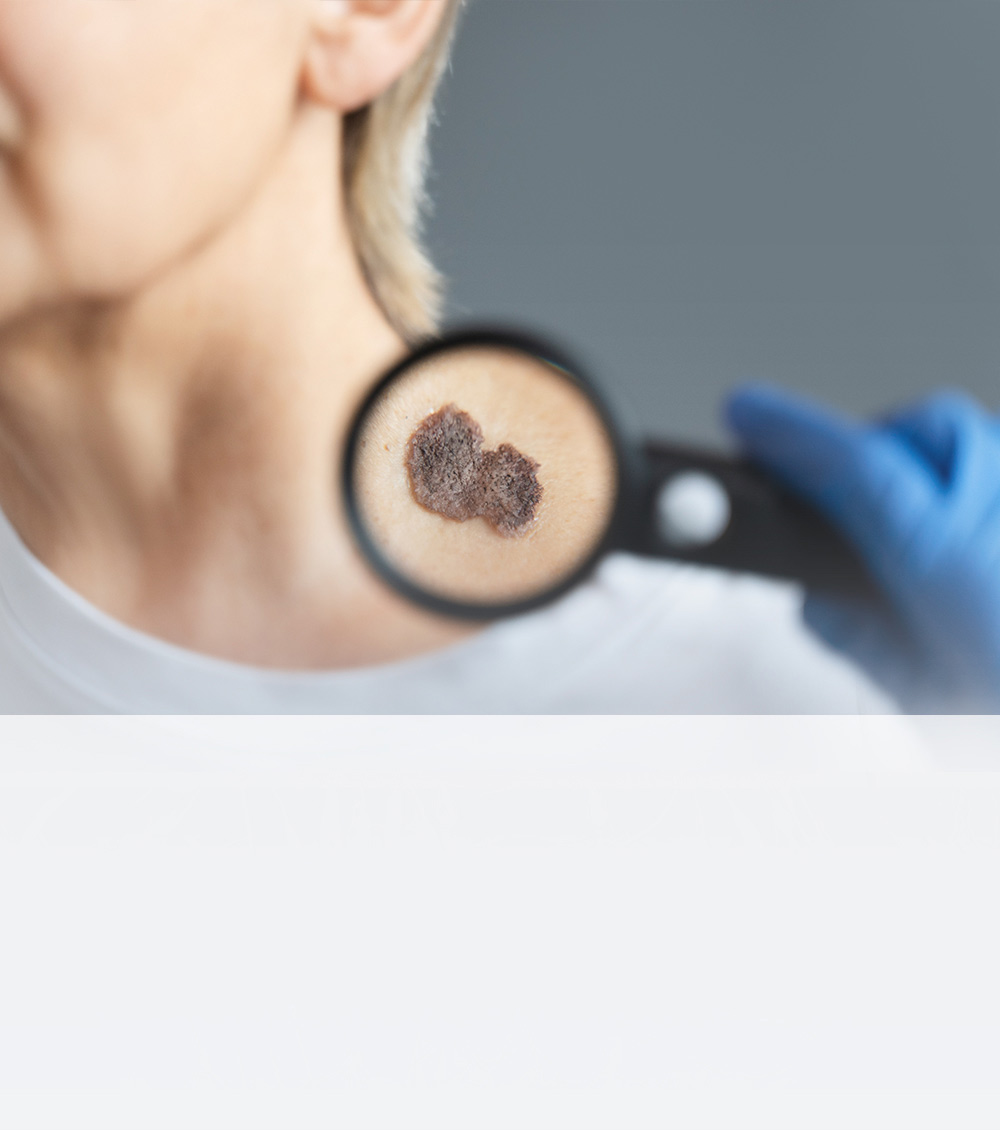
Types of Skin Cancer
There are the following types of cancer:
- Basal cell carcinoma: This cancer develops in the lowermost layer of the epidermis and usually occurs in skin regions exposed to UV rays. These cancers grow slowly and are less likely to metastasize to other parts of the body with higher chances of making a recurrence.
- Squamous cell carcinoma: These account for almost 20% of non-melanoma cancers of the skin. Squamous cells are the flat cells on the outermost layer of the skin and are more likely to be found in areas exposed to the sun like the head, neck or arms. They usually metastasize to surrounding lymph nodes and if left untreated spread to distant organs as well.
- Melanoma: Malignant transformation of melanocytes gives rise to melanoma and is aggressive. Melanocytes are the skin cells responsible for producing melanin; a pigment accountable for skin colour, which protects us from the UV rays. These cells darken (as they release more melanin) on exposure to the sun as a response to protect the skin from the harmful effects of UV rays.
- Merkel cell carcinoma: This is an aggressive form of cancer that originates in the Merkel cells, which are responsible for touch sensation. They are typically common in areas like the head, scalp or face, with the tendency to metastasize to the brain, bones, liver and/or lungs
- Rare skin cancers:These include Kaposi’s sarcoma, sebaceous gland carcinoma, cutaneous lymphoma etc.
Prevention of Skin Cancer
Tests for Skin Cancer:
- Incisional biopsy:a small sample is taken after administering local anaesthesia and sent for histopathological reporting.
- Excisional biopsy: for smaller growths or suspicious areas, the entire area is removed under local anaesthesia.

Treatment includes
Surgery
Non-surgical options include:
Doctors

Dr. Sachin Chavre

Dr. Aruna Prabhu

Dr. Karthick Rajamanickam